Historically, breast cancer has been viewed as a disease of aging. However, recent epidemiological data has signaled a concerning shift: the incidence of breast cancer in women under the age of 50, particularly those in their 20s and 30s is on the rise. While still relatively rare compared to cases in postmenopausal women, the increasing frequency and the often aggressive nature of early-onset breast cancer have made this a critical focal point for medical research and public health.
Understanding why this is happening requires looking beyond simple statistics. It involves a complex interplay of shifting societal norms, environmental exposures, and biological drivers that make breast cancer in young women a distinct clinical challenge.
The Statistical Reality: A Growing Trend
Recent reports from major cancer registries indicate a steady upward tick in early-onset breast cancer cases. While overall breast cancer mortality has decreased due to better treatments, the rate of new diagnoses in women under 40 has increased by approximately 1% to 2% annually over the last decade.
In young women, these cancers are more likely to be diagnosed at a later stage, often because neither the patient nor the physician immediately suspects cancer in someone so young. Furthermore, the biology of these tumors tends to be more aggressive, with a higher prevalence of Triple-Negative Breast Cancer (TNBC) and HER2-positive subtypes compared to older populations.
The Role of Reproductive Shifts
One of the primary drivers cited by researchers is the change in reproductive patterns over the last several decades. Biological protection against breast cancer is often linked to the total number of menstrual cycles a woman experiences in her lifetime.
- Delayed Childbearing: Having a first full-term pregnancy before age 30 is known to have a long-term protective effect on breast tissue. As more women delay childbirth into their 30s or 40s, or choose not to have children, they lack this hormonal reset.
- Early Menarche: The age at which girls experience their first period has been dropping globally. Longer lifetime exposure to estrogen and progesterone, the hormones that can fuel certain types of breast cancer increases the cumulative risk.
- Reduced Breastfeeding: Breastfeeding for a cumulative period (usually 12 months or more) reduces risk by pausing ovulation and maturing ductal cells. Lower rates of breastfeeding in some populations contribute to the risk profile.
Environmental and Lifestyle Catalysts
Modern life has introduced a suite of silent risk factors that disproportionately affect younger generations who have been exposed to them since birth.
The Impact of Metabolic Health
Obesity and physical inactivity are well-documented risk factors. Adipose tissue (fat) acts as a metabolic organ, producing estrogen and inflammatory cytokines. In younger women, high levels of insulin and insulin-like growth factors (IGF) can promote the rapid division of cells, potentially leading to malignancy.
Endocrine Disruptors
We live in an era of forever chemicals. Bisphenol A (BPA), phthalates, and certain pesticides found in plastics and personal care products are known as endocrine-disrupting chemicals (EDCs). These substances can mimic estrogen in the body, binding to receptors and interfering with normal hormonal signaling during critical windows of breast development, such as puberty or pregnancy.
The Biological Distinction: Why Young Cancers are Different
Breast cancer in a 30-year-old is not the same as breast cancer in a 70-year-old. On a molecular level, tumors in younger women are often more plastic and resistant to standard therapies.
Genomic Mutations: While BRCA1 and BRCA2 mutations are more common in younger patients, many cases occur in women without a known family history. Researchers are investigating de novo mutations genetic changes that occur during a person’s lifetime rather than being inherited.
The Microenvironment: The breast tissue of a young woman is denser and more immunologically active. This can sometimes create a fertile soil for cancer cells to hide and grow, making them harder to detect on standard mammograms.
The Challenge of Detection and Screening
The standard recommendation for mammograms often begins at age 40 or 45. For a woman in her 20s or 30s, this means there is no routine screening protocol.
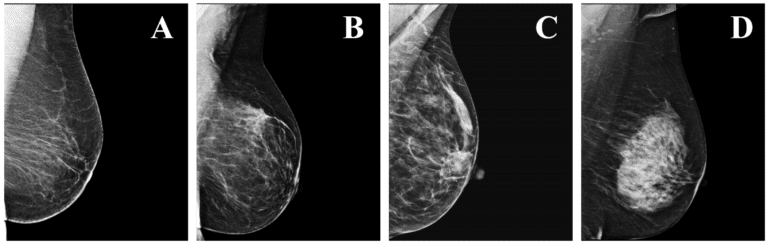
- Dense Breast Tissue: Younger women typically have dense breast tissue, which appears white on a mammogram the same color as a potential tumor. This makes mammography less effective for this age group.
- The Too Young Bias: Many young women who discover a lump are told it is likely a benign cyst or a fibroadenoma. While this is often true, the delay in diagnostic imaging (like ultrasound or MRI) can allow an aggressive cancer to progress.
Actionable Steps: Prevention and Advocacy
While we cannot control our genetics or the age of our first period, there are significant ways young women can manage their risk and advocate for their health. 
Know Your Normal
Breast self-awareness is key. You don’t need a formal exam technique, but you should know how your breasts look and feel throughout your cycle. If you notice a persistent change, a lump, skin dimpling, nipple discharge, or redness insist on an ultrasound.
Genetic Counseling
If you have a family history of breast, ovarian, or pancreatic cancer, don’t wait until you’re older to seek genetic counseling. Knowing your status early allows for high-risk screening protocols, such as annual MRIs, which are much more sensitive than mammograms.
Metabolic Maintenance
Focusing on a Mediterranean-style diet, limiting alcohol, and maintaining consistent physical activity can help regulate insulin and estrogen levels, providing a degree of internal protection.
A Call for Early Awareness
The rising incidence of breast cancer in young women is a sobering reminder that youth is not a shield against the disease. The rising risk is a product of our environment, our changing lifestyles, and the complex biology of the modern age.
By shifting the conversation from “it won’t happen to me” to “I know my body and my risks,” we can catch these cases earlier when they are most treatable. Science is moving fast, with new genomic therapies and better imaging, but the most powerful tool remains the informed and proactive patient.
If you feel something, say something. Don’t stop until you have an answer.